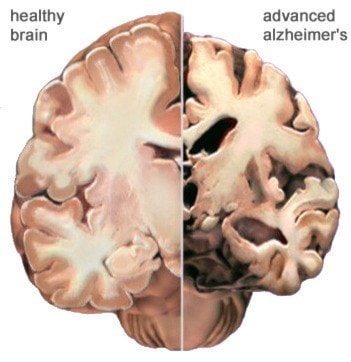
Understanding Alzheimer's disease and dementia starts with the basics: what exactly is the difference between the two?
The main difference is in the title. Dementia is not a disease, but rather a large class of brain disorders that affect thinking ability and memory, according to the Alzheimer's Society of Canada's "hope.courage.progress" report released in October, 2011.
Alzheimer's disease is the most common of the dementias, but there are many others. Some dementias are reversible, simply by a change in diet. But others like Alzheimer's are progressive and do not have a cure, and are so named irreversible dementias.
Alzheimer's accounts for about 60 to 80 per cent of diagnosed dementia cases. The second most common type is Vascular dementia, which occurs after a stroke.
Memory loss does not always mean dementia has set in, and visiting a physician can help a patient discover what the true cause is. For a dementia diagnosis, a patient must exhibit one of two impairments to mental functions including memory, communication and language, ability to focus and pay attention, reasoning and judgement and visual perception.
Dementia is caused by damage to brain cells. In Alzheimer's specifically, nerve cells in the brain become sick and are less and less capable of passing on messages to other cells. Eventually they die off and the loss of connectivity is what causes cognitive decline. As the brain cells die, the brain shrinks, starting with the thinking and memory portions of the brain. It eventually spreads and affects most areas of the brain.
Memory is not always the first thing that caregivers notice before their loved one is diagnosed with a dementia —but it can be one of the most difficult symptoms for family to deal with. In advanced stages of Alzheimer's, the patient may not recognize loved ones at all.
A red flag is when a loved one begins to repeat what they just said minutes earlier, or when lapses in judgement affect paying bills or other common tasks.
Alzheimer's patients can also have personality changes. They can become agitated, aggressive, depressed and experience paranoia, although this is not always the case. Another big worry for families is that Alzheimer's patients will often wander and can become lost in usually familiar areas.
Once the disease progresses, the person may become unable to take care of themselves, which puts further strain on caregivers. According to the Alzheimer's Society of Canada report, the disease is ultimately fatal. Death is caused by inactivity, loss of appetite, muscle wasting, a reluctance or inability to cough and a compromised immune system. Pneumonia is common in end-of-life Alzheimer's patients because of the impaired immune system and generally occurs between seven and 10 years after diagnosis.
Many younger caregivers wonder if their parent has Alzheimer's if the disease will be passed on to them as well. The Alzheimer's Society of Canada report says that is not always the case, as only one of two types of Alzheimer's is genetic.
"Actually, having a direct relative with Alzheimer's disease does indeed increase one's own risk of getting it, by some three times," The report reads. "Before becoming too pessimistic about genetic susceptibility, however, it is important to see what a threefold increase actually means."
The report explains that on average, five out of every 100 people aged 65 will get Alzheimer's disease and 95 people will not. With a threefold increase, those rates change to 15 in every 100, meaning 85 people will not.
"The extra risk of having an affected direct relative is not so huge after all," the report says.
The other obvious risk is aging itself. The Alzheimer's Society of Canada report says that while particular risks have been identified to potentially increase the risk of dementias, there is little scientific evidence to explain the links. Those potential risks that could increase the chance of being diagnosed with Alzheimer's later in life include diabetes, head injury, irregular heart beat, lack of physical exercise, Down Syndrome and clinical depression.
See tomorrow's Townsman/Bulletin for more in this series on dementia and Alzheimer's disease to mark Alzheimer's Awareness Month. We will look at ways to prevent dementia, treatment options for those diagnosed, responsibility of caregivers and more.